| |
Practice ManagerDiary Administration- Organise competent personnel to complete the day’s workload.
- Confirm all changes that have been made in the practice have also been implemented on the system.
- Manage user access control.
- Ensure all practitioners have been created on the system.
- Confirm that diaries have been created for the practitioner and practice.
Debtors & Patients- Ensure that Reception checks all information.
- Double-check that all patients have electronic files.
- Ensure there are knowledgeable personnel available at reception to open files on a daily basis.
- Decide when electronic record update requests should be sent to ensure correct and updated patient information.
Appointments- Ensure that all information is in the diary so that anyone can manage the day-to-day bookings regardless of the availability of specific personnel.
- Manage the waiting room and the time patients wait for consultations.
- Check the diary to see if all documents have been uploaded onto the software, all necessary processes were completed, all theatre lists were sent to hospitals, and all correct information was added for the next day.
Communication- Ensures that all communication to and from patients and all internal communication is responded to.
- Complete all tasks and ensure all tasks of other personnel are done.
Billing & Corrections- Design and check the process to get files and billing notes from the Practitioner to the Billing Expert and check that all billing is daily up to date.
- Ensure the prices on the system is always up to date.
- Adjust private rates on the system when the practice increases/changes prices.
- Ensure that corrections are done by authorised personnel by utilising the correct functions in the software.
- Check all corrections daily and weekly to ensure no unauthorised or unnecessary corrections are made.
- Ensure that only authorised personnel have access to do corrections.
Claim Administration- Check that all claims were sent before the end of the business day.
- Ensure all rejections have been dealt with daily.
- Ensure no “To be sent" or “flagged for submission" claims exist.
- Ensure the Billing Expert and Credit Controller relationship is in place and maintain proper communication between them.
Receipting & Corrections- Check the cash and card reconciliations daily.
- Ensure the correct personnel are responsible for banking the cash.
- Allocate the right cash to petty cash if the money is used for day-to-day expenses.
- Investigate any discrepancies when reconciliation is not complete or does not reconcile.
- Ensure that all ERAs are posted and balanced with the bank account.
- The Practice Manager can write incorrect receipts back.
Debt Management- Ensure that notes on the Age Analysis are updated.
- Approve journals.
- Approve and check that all information is accurate on accounts to be handed over for debt collection.
- Ensure that the practice receives feedback on accounts handed over for debt collection.
Reports & Internal Controls- Ensure all transactions are current before reports are generated and sent to management.
- Draw and check all reports and send them with notes (if needed) to the responsible manager(s).
- Implement management decisions to optimise operations.
|
| |
Receptionist
Diary Administration- Daily management of all available time slots on all diaries for all Practitioners.
- Confirms that the correct configuration is done on all diaries for the day-to-day functions to create an optimal workflow.
Debtors & Patients- Open electronic files of Debtors and Patients, upload all required documents and ensure the correct demographic details of debtors and patients are on the system.
- Do validations and benefit checks before consultations.
- When dependants are deceased, acquire their own medical schemes or duplicate files are mistakenly opened, they must be marked inactive and/or moved to their own electronic files.
- Ensure all revised documents are electronically updated and available.
- Ensure all electronic record update request responses have been accepted or rejected.
Appointments- Complete all bookings for prior telephonic appointments, walk-in patients and online bookings.
- Manage all changes in bookings. Move, extend and cancel appointments.
- When appointments are cancelled, ensure that the Waiting List is managed.
- Ensure all demographic information is correct and updated.
- Compile the theatre list, schedule patients on the theatre list and complete all pertinent information.
- Follow up on bookings beforehand.
Communication- Ensure all communication is responded to and all tasks are completed.
- Send SMS reminders for patients to remember appointments.
- Send birthday wishes to Patients and ensure all documentation is uploaded and updated.
|
| |
Billing Expert
Communication- Check all tasks daily.
- Ensure all communication from the Practitioner was received, understood and completed.
- Ensure the practitioner will communicate the billing codes that should be billed, for example, by email, tasks, clinical events or the episode manager.
Billing & Corrections- The Billing Expert must have advanced knowledge of the speciality’s billing codes and rules to ensure accurate and optimal billing.
- Ensure all medical scheme billing is switched to the medical schemes and all corrections are done.
- All billing must be done daily to ensure correct figures and healthy cash flow.
- Private patient billing must preferably be done before the patient leaves the practice, so the need for debt collection is limited.
- Will process all billing corrections, for example, Credit Notes, Redo Transactions and Edit Invoice functions. Utilises the appropriate functions for the different types of billing errors.
Claim Administration- Use validations and imported data to prevent rejections.
- Ensure all claims are sent daily.
- Follow up on all rejected claims or line items on the claims, make corrections, and resend claims to medical schemes. Complete the 4 R’s: Reverse, Redo, Resend, Resolve.
- Ensure all claims are dealt with and that Approved-in-full claims are resolved to update the list, which the Credit Controller uses to follow up on outstanding claims.
|
| |
Cashier
Receipting & Corrections- Receive all Patient payments by card and cash.
- The Cashier must allocate the payments to the correct accounts and print receipts for the patients where required.
- All cash and card payments must be reconciled daily.
- Bank the cash that was received for a certain period.
- When money is used for day-to-day expenses, it must be given to the Practice Manager and allocated to the Petty Cash cash book before it is used for daily expenses.
- Link all payments to the corresponding invoices.
- When errors occur, corrections must be requested from the Practice Manager or Credit Controller (Receipt Written Back).
|
| |
Credit Controller
Communication- Use SMS, email, and VOIP calls to communicate with Patients with outstanding accounts.
- All communication between the credit controller and the medical scheme or patient must be documented.
- Complete all tasks.
Billing & Corrections- Check that all billing and corrections were done and all medical scheme claims and corrections were submitted.
- Ensure that all outstanding invoices are sent as soon as possible to patients.
- Check that all billing and corrections were done and all medical scheme claims and corrections were submitted.
- Ensure that all outstanding invoices are sent timely to patients.
Claim Administration- Ensure all possible methods are used to correct claims, and all claims are sent to medical schemes.
- Ensure medical schemes receive all claims so that payment can be obtained with the next payment run of the medical schemes.
- Ensure correct claims are marked as resolved, and those not resolved are flagged for debt collection.
Receipting & Corrections- Allocate EFT payments to the correct patient accounts.
- ERAs must be posted daily but only when the amount is visible on the practice’s bank statements.
- ERAs that have not yet been received into the practice's bank account should not be posted; otherwise, there will be no reminder to follow up on payments with medical schemes that have not been paid.
- Complete receipt corrections. The Practice Manager or the Credit Controller can perform this task.
Debt Management- Follow a pre-designed debt collection cycle by completing tasks in each stage.
- Make notes, create daily tasks, and follow up on those tasks: contact medical schemes and private patients for outstanding accounts.
- Accounts of 60+ days or older are URGENT accounts and must be dealt with immediately.
- Collect as many outstanding accounts as soon as possible to ensure healthy cash flow in the practice.
- Hand over outstanding accounts for formal debt collection.
- Journals must be posted to the correct Ledger accounts.
- Send outstanding patient accounts by email or SMS.
|
| |
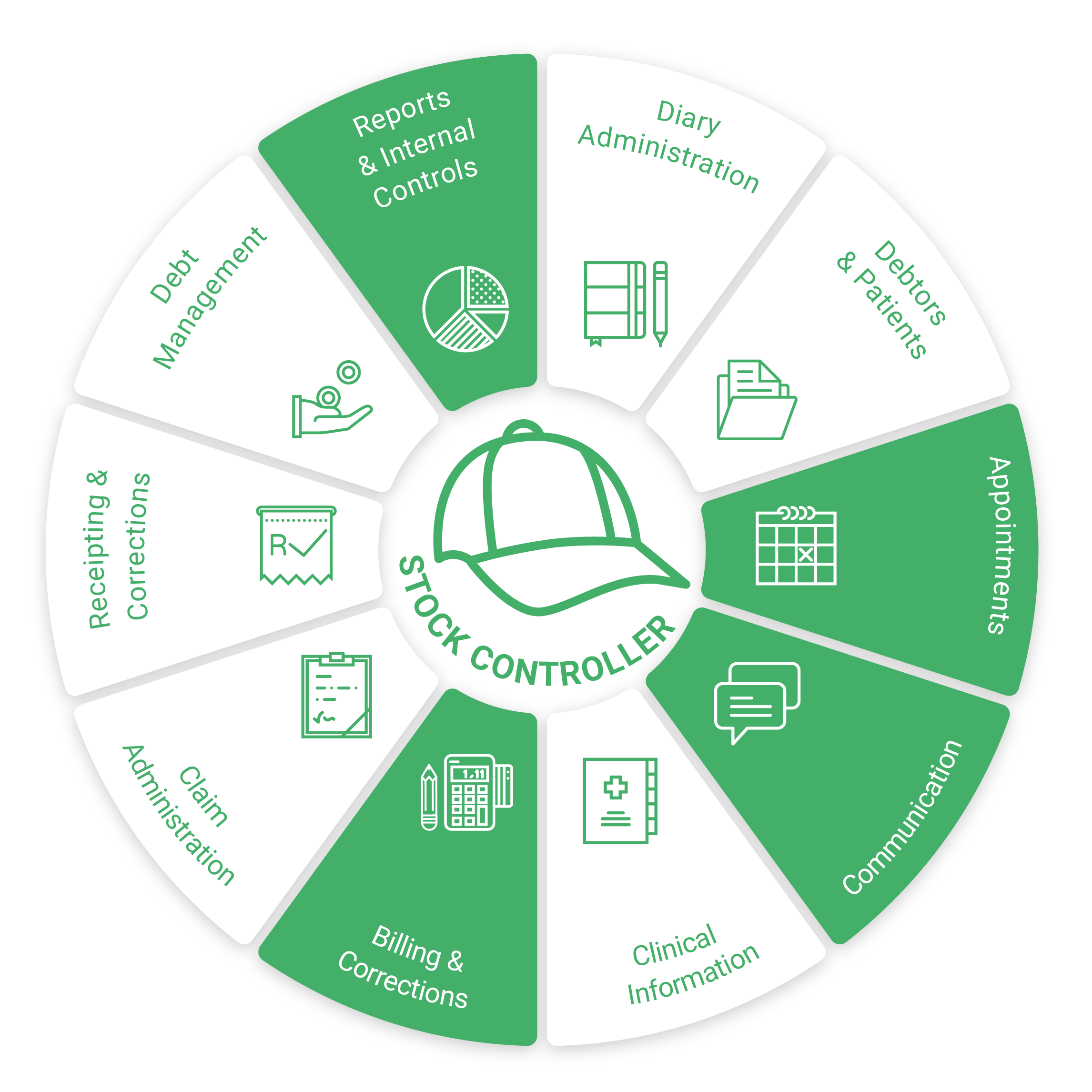
Stock Controller
Appointments- Check patient bookings to ensure that the practice has enough stock to treat the number of patients booked for a certain period plus the number of patients that the practice has the capacity to still book for that period. (The reason for the appointment can be an indicator of the specific items that will be needed.)
- Go through all the chronic patients to ensure the stock will be ready for the patients to be collected.
Communication- Use Minimum & Maximum stock levels report daily to see if any stock should be ordered from Suppliers.
- Send orders to suppliers with the correct item information.
- Check tasks to ensure all instructions from Practitioners are completed.
Billing & Corrections- Check all billed stock and ensure all used stock is billed.
- Mark all stock items that will not be charged as non-chargeable.
- Check that used non-chargeable items are billed to patient accounts or a non-chargeable account.
- Check that the correct item, strength and pack size were used with the billing. Confirm that the cost of sales has been calculated and is accurate. Ensure there is stock to be billed and all supplier invoices are current.
- Check that applicable corrections were made. (Credit notes will affect the stock levels, but journals not.)
- Ensure credit notes were made when the stock was returned or not used on patients.
Reports & Internal Controls- Check the audit trail to ensure the correct stock was billed.
- More reports will be used in stock management to provide the correct details.
|
| |
Bookkeeper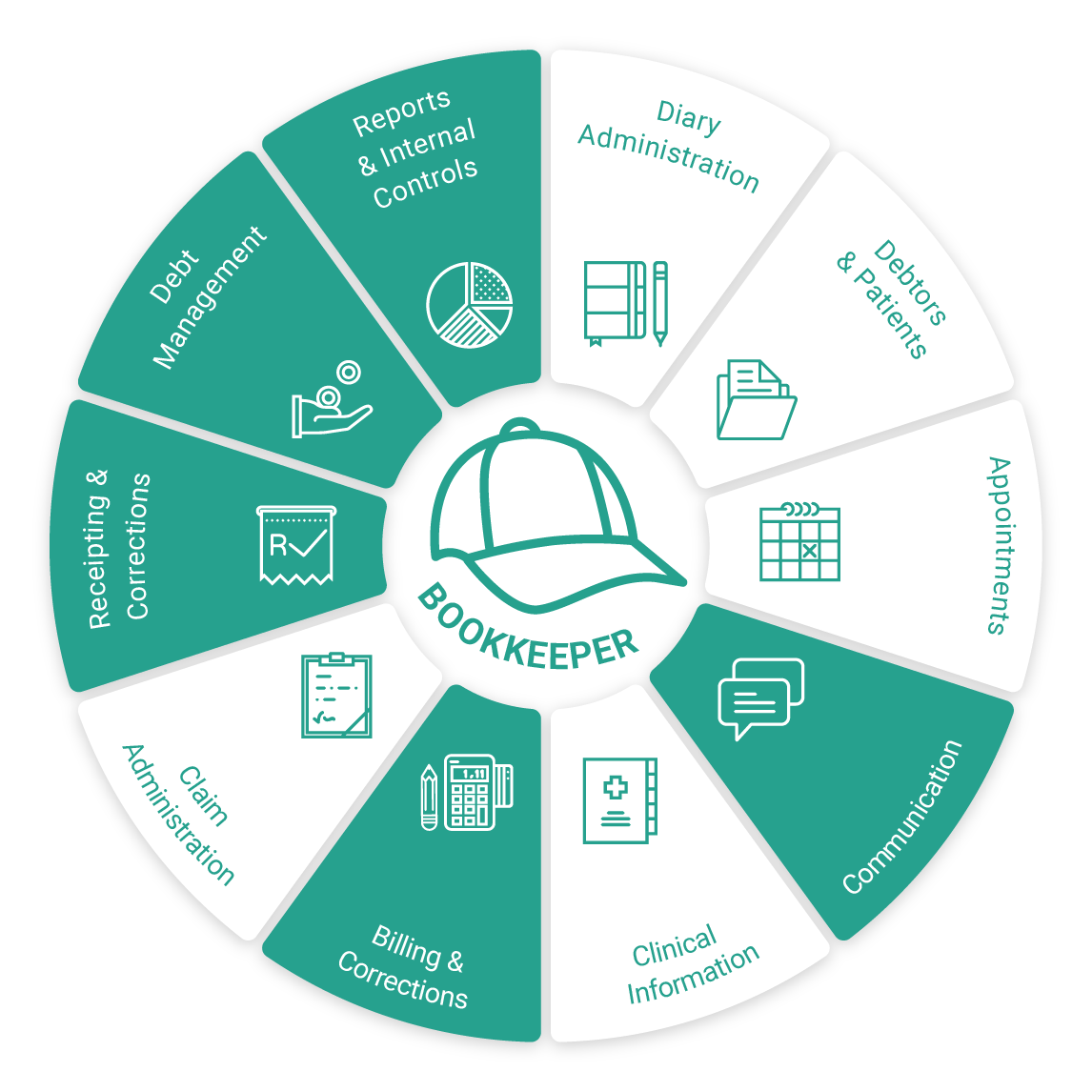
Communication- Collaborate with auditors about the financials of the practice.
- Send reports to the Auditors for the financial reports to be compiled and audited before being submitted to SARS.
- Submit reports & payments to SARS and handle queries.
Billing & Corrections- Ensure that billing was done correctly and balances with the Audit Trail.
- Ensure that VAT calculations are correct.
- Draw reports to check that corrections are annotated with the right reasons and that only authorised personnel have access to corrections.
Receipting & Corrections
- Draw the list with the reasons for all the receipt corrections (Receipt Written Back).
- Check if proper reasons were given and if authorised personnel did the corrections.
Debt Management- Investigate the Age Analysis report regularly.
- Ensure that the Credit Controller followed up on outstanding accounts and accounts were handed over correctly.
- Ensure that correct journals are done and documentation is correct.
Reports & Internal Controls- Check all reports, and ensure all reports balance and the information on the reports is correct.
- Send reports to the Auditors for the financial reports to be compiled and audited before being submitted to SARS.
|